Georgia Vasectomy Reversal | Experience, Success and the Best All-Inclusive Price in the Southeast.
Microscopic Vasectomy Reversal Urologist | Dr. McHugh is one of southeast’s most experienced microscopic vasectomy reversal specialists. Significantly, Dr. McHugh performs reversals weekly in our practice owned and accredited surgery center.

Microscopic Vasectomy Reversal Urologist | Surprisingly, few urologists perform vasectomy reversals and even fewer perform commonly.
In fact, it is rare for any urologist to perform vasectomy reversals on a weekly basis.
Why Is That?
- There is a steep learning curve to master. A microscopic vasectomy reversal is difficult to perform.
- The ability to provide the necessary components to perform microscopic vasectomies is expensive.
- Very view of the patients who have a vasectomy want to reverse it (5%). Active reversal surgeons draw their patients from a large market area.
- A reversal is not covered by insurance.
- Success is not guaranteed.
- Having to use a hospital increases the cost dramatically and performing in an office limits the type and level of anesthesia offered.
- The procedure takes 2-4 hours to perform.

Why is the skill in using an operating microscope and having an experienced surgeon reverse your vasectomy important?
Interestingly, the answer is complicated. Below detail several of the reasons. Notably, only 5% of the men who have had a vasectomy will desire to reverse it. As a result, this limits the number of patients who need a reversal. Furthermore, most urologists uncommonly see patients who need a reversal.
Additionally, insurance does not cover a vasectomy reversal. The surgeon offers a package plan for all of the costs involved. In other words, the surgeon coordinates, and pays the various entities necessay to perform a reversal.
Incidentally, Dr. McHugh utilizes an operating microscope and uses microscopic suture to join the very small openings. Additionally, he places 14-16 sutures in each vas deferens.
For example, the thickness of a strand of hair is 100 microns.
Moreover, the surgeon operates with suture measuring 70 – 100 microns. Therefore, the suture is about the diameter of the human hair.
Of note, the outside thickness of the vas deferens is about 2 mm. The lumen of the vas (the inner channel) averages about 5.6mm in diameter.
In addition, 500 microns is about the size of the opening in the vas deferens (.5mm).

As a matter of fact, the lumen of the vas deferens is approximately the size of the “O” in God on a penny.
Interestingly, Dr. McHugh places 14-16 microscopic sutures the size of hair to join a tube that is less than a millimeter in diameter.
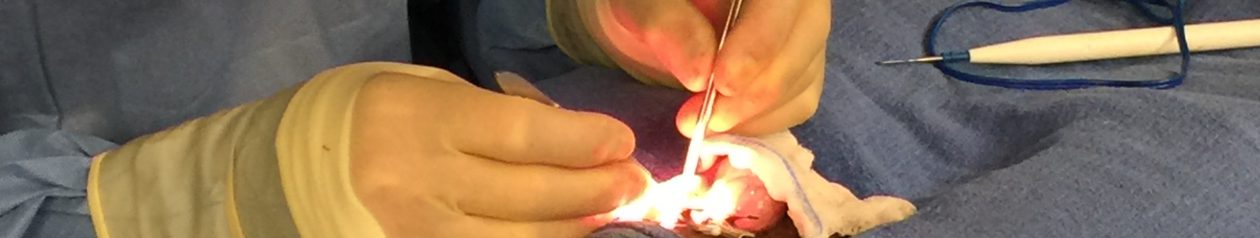
Microscopic Vasectomy Reversal Urologist

- Note the microscopic needle at the top of the image.
- The vas deferens lumen (opening ) is seen in the center of picture.
- Microscopic black sutures are shown traversing the two ends of the vas in preparation for closing the repair. (Look closely, you’ll see them!)
Notably, surgeons use suture to close an incision of any common non-microscopic surgical procedure that is bigger than the tube in which sperm travels in the vas deferens. Hence, the necessity of microscopic suture.
In summary, reversal surgeons use very small sutures to connect very small openings. In other words, there has to be enough room after connecting the tubes for sperm to travel in their quest to achieve pregnancy.
Contact Us.
Vasectomies and Vasectomy Reversals performed by Dr. McHugh since 2020!
Vasectomies
Vas Reversals
Vasectomies and Reversals


Few Urologists Perform Microscopic Vasectomy Reversals | In short, the necessary components of a successful vasectomy reversal practice:
✅ Experienced and skilled microscopic surgeon. Dr. McHugh has performed hundreds of microscopic vasectomy reversals.
✅ Practice owned and nationally accredited surgery center. This assures safety, oversight and the ability to offer general anesthesia.
✅ Success. See some of our success stories.
✅ Acceptable all-inclusive price with no hidden fees. See breakdown of cost package.
✅ Board Certified: American Board of Urology.
✅ Experienced staff (R.N.s), operative microscope, microscopic instruments and sutures.
✅ Awarded “Best in Georgia.” Dr. McHugh is one of the southeast’s most experienced microscopic vasectomy reversal specialists.
✅ Performs vasectomy reversals on a regular basis. Dr. McHugh does two reversals each week.
✅ Informative website with content written by Dr.McHugh based on personal experience and national studies. See In link bio|Dr. McHugh
✅ Free and convenient vasectomy reversal phone consultation.
Common Vasectomy Reversal Questions:
- What is the success rate? This depends on the experience of the surgeon, the interval of time between the vasectomy and the reversal and the findings at the time of the surgery. The shorter the interval the better the chances of success. Success rates-Click here.
- How many microscopic vasectomy reversals has Dr. McHugh done? Thousand of procedures and hundreds of vasectomy reversals have been successfully performed in our accredited Urological Surgery Center.
- What is the cost? Our fee is all-inclusive and “no hidden fees.” (Surgeon fee, Accredited Facility Expense, Anesthesia, R.N. nursing, Operative microscope, microscopic suture and… an experienced, skilled and pleasant staff.)
In fact, Dr. McHugh performs two reversals every week in our practice owned and accredited surgery center.
- Importantly, we perform microscopic vasectomy reversals on a weekly basis in our practice owned, accredited for general anesthesia and dedicated reversal facility.
- Do you have a payment program? Yes, we are in network with CareCredit.com for this option.
- Will I have any pain during the procedure? No, we provide anesthesia by a board certified anesthesiologist. Our safety record has been impeccable. The pain after the procedure is slightly more than you may have experienced during the vasectomy.
- Is it like having a vasectomy? No, a vasectomy takes 15 minutes and done through a “size of rice” opening. A vasectomy reversal takes our team approximately 2 hours. As a result, one can expect a bit more swelling and bruising. “The procedure involves the same tube… but it’s a different operation!”
- Is the age of my wife important? Yes. Success rates begin to decline as the female’s age goes above 39. The male is less age dependent.
What’s more, we include hotel accommodations in our all-inclusive cost.
- What if I have to travel a long distance to go home? Most couples will arrive the day of the procedure and then spend the night afterwards in a local hotel. Hotel accommodations if necessary is complimentary for one night. (As a rule, couples within a few hours drive from our facility prefer to go home after the procedure and this is acceptable.)
- How long before I can drive? Usually within a week. If the surgery is on a Thursday, for instance, the longer you can be off your feet with the scrotum elevated the less swelling you will experience. The complete healing doesn’t occur until around a month, but patients can be active but careful during that time. Tight compression exercise underwear is better than the traditional “jock support.”
After the Vasectomy Reversal Common Questions
- When can I resume sexual activity? In three weeks.
- When can I return to work? Desk work, with caution and being careful, in one week. If one has a strenuous job usually three weeks, however a lot of patients go back in one week but they have made arrangements to gradually get back to their normal work routine. (With the help of their co-workers.)
Importantly, Patience is a virtue.
- How long does it take for the testicles to produce sperm again? Usually 4-6 months depending on when the vasectomy was done. (The shorter the interval between the reversal and vasectomy, the sooner the vesicles begin to produce sperm.)
- If pregnancy occurs, what is the most common time frame? 6-18 months. This is important to remember this as achieving pregnancy after a vasectomy reversal is a patient process.
Moreover, opportunities for earlier booking is often available for patients choosing to be added to our active waiting list.
- Are birth defects more common after a vasectomy reversal? No.
- Which is better in vitro methods or a vasectomy reversal? This is a decision which the couple should research and based on what is best for them. Proponents of a reversal state cost, the ability to have more than one pregnancy, less requirements by the female, and a more streamlined process from the decision to having the procedure.
- How soon can I schedule the procedure? It is unusual not to be able to schedule within a 6-8 weeks of inquiring. Our practice owns our surgery center, so it is not uncommon to open another operative day and perform two reversals on the same day to accommodate demand. (We also have an active “Waiting list” for couples who want to have the procedure sooner and are zable to be available on short notice.)
Importantly, in the vast majority of cases the pre-operative medical evaluation and consultation can be done over the phone.
- Is it necessary to have an in person consultation visit? In most cases no. The anesthesia doctors do not require new blood work or EKG if the patient is less than 50 and not on certain medications. The only thing that can’t be done ahead of the procedure is the exam of the testicles.
- Is there a safety risk of the procedure or of the anesthesia? It is rare to have any injury to the testicles. Infections are uncommon, bruising is common. There is no change in the male sexuality. The anesthesia is very safe and to date we have had no issues/complication related to this. Our anesthesiologists are all certified. Our safety record has been impeccable since opening our facility in 2008.
- Dr. McHugh only performs no scalpel vasectomies and microscopic vasectomy reversals. Dedicated pages: Northeast Georgia Urology, Georgia Vasectomy Reversal Center, and Georgia Vasectomy Reversal.
In summary, the vasectomy reversal requires many components to come together for the desired outcome. The precious addition to your family.