Best of Georgia Vasectomy Reversal | Success, Experience and the Best All-Inclusive Package Cost in the Southeast.
John C. McHugh M.D.
Top Vasectomy Reversal Surgeon in Georgia |Best in Georgia Award
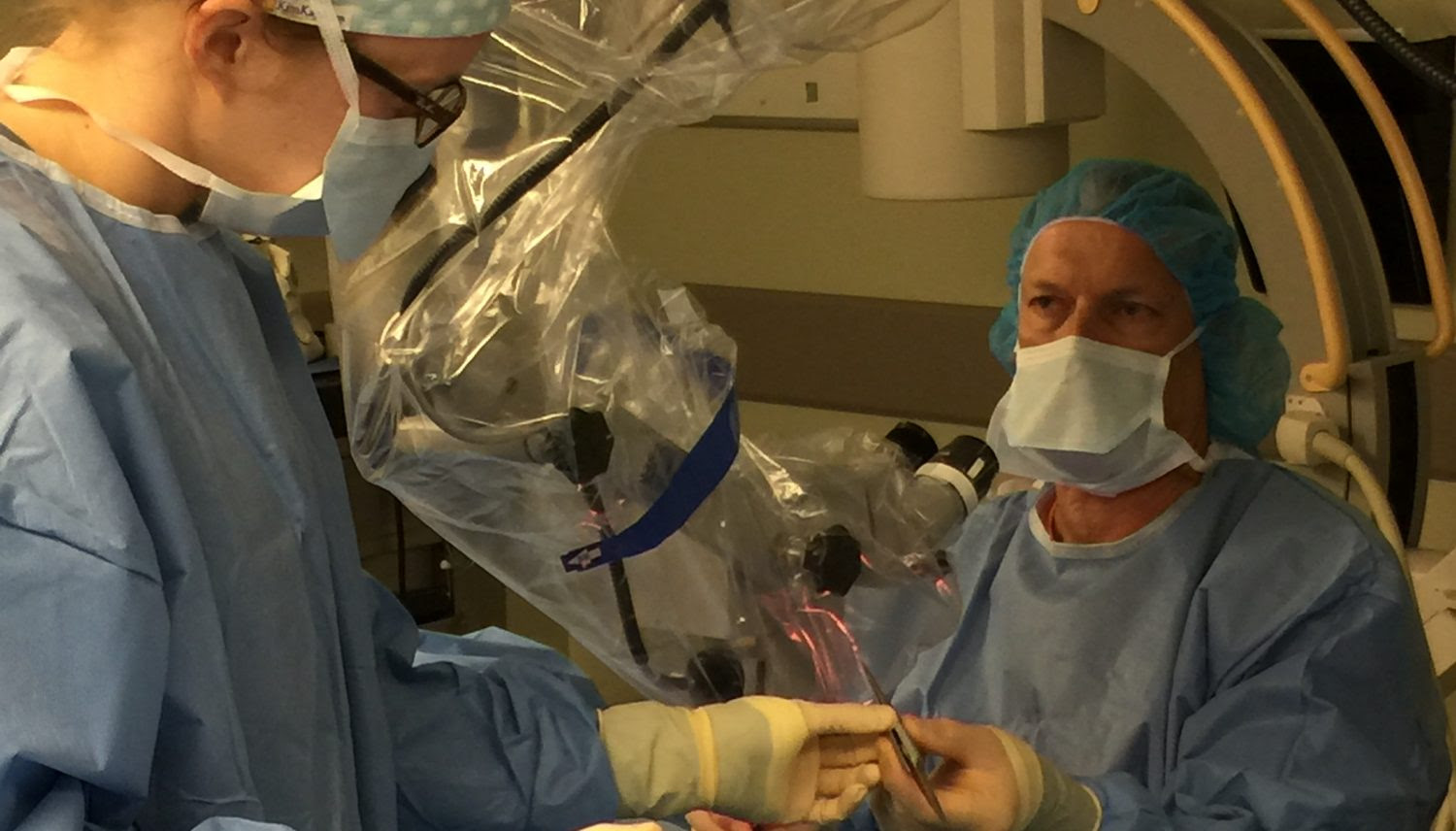
Dr. McHugh specializes in microscopic vasectomy reversal. He is one of the Southeast’s most experienced microscopic vasectomy reversal urologists. He utilizes a Zeiss operating microscope with microscopic instruments and sutures.
Vasectomy reversals are performed in his practice owned and accredited urological surgery center with anesthesia provided by board certified anesthesiologists. Over 500 microscopic vasectomy reversals have been performed in our surgery center since 2008.
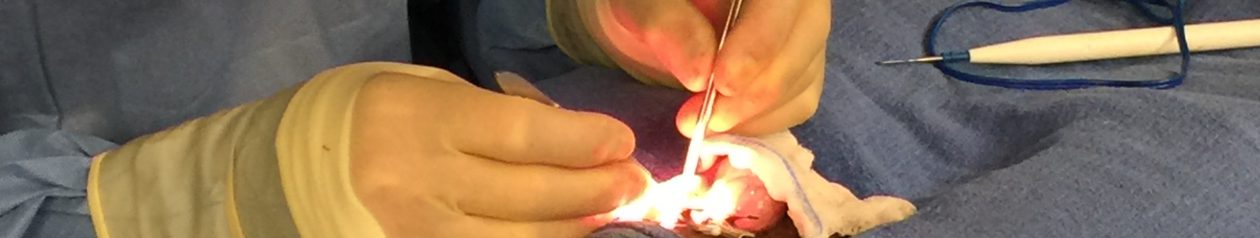
Vasectomy Reversal Technique

Using an operating microscope, suture the size of hair (9-0 Nylon) is used to align the lumen of the vas tubes. Dr. McHugh uses the Modified Two-Layer technique. The first layer joins both the outside of the vas and the lumen (the channel that carries the sperm).
The second layer joins the outside of each of the vas tubes. This method provides for both the proper alignment of the lumen as well as support of the repair ensuring a tension free anastomosis.
Studies have shown that this technique has similar success rates as other methods which take longer to perform and can incur a greater expense. A total of 12-14 sutures are placed on each side and as a result the procedure generally lasts two hours. The entire time spent at our facility is usually around 3 hours.
Contact Us!
Phone: 770-535-0000
Email: jmchugh@gavasectomyrevesal.com
Contact Form: Try it…we respond promptly!
Vasectomy Consults are Scheduled As Office Visit
Vasectomy Reversals (Most patients are hours away) – Phone Consultations are Complemenatry
Consultationa can be arranged by phone or contact form.