Tag Archives: vasectomy reversal
Common questions about a vasectomy reversal answered by Dr. McHugh on Vasectomy.com
Intimacy after vasectomy same as after a vasectomy reversal?

From Vasectomy.com
I usually tell patients wait one week after a vasectomy and three weeks after a vasectomy reversal before resuming sexual activity. Other than the fact that the reversal is a more substantial procedure to recover from in time there is little difference in this particular regard. JM
FAQ-Vasectomy Reversal
Question: The patient has had a vasectomy and has only one testicle. Can you achieve pregnancy with only one testicle?

The question on vasectomy.com is about IVF however a microscopic reversal is also a reasonable option in this scenario.
It takes two to tango but only one testicle to conceive!
How long out of work if you have a vasectomy reversal? Ga Vasectomy Reversal.
Medical aphorism: “The art of getting away with it.”
Patients who are considering a vasectomy reversal usually have a busy life. They to a person don’t like being out of work and even if they did their employer probably won’t view a reversal as medically necessary. So a common question is how soon can I go back to work and how soon to resume working out? Well…this is where “getting away with it” comes in.
Since a reversal is a procedure which usually takes a bit over two hours, the incision on each side is open for about an hour each and this lends itself to bruising and scrotal swelling. A patient can physically go back to work in three to four days but because of the nature of the procedure and the fact that the scrotum is a dependent structure (hangs down) and is potential space (not tight like the skin over your arm) it is prone to bruising and swelling.
So the answer…you can “get away with” three to four days but:
- The longer you are off your feet and elevate the scrotum the less swelling and bruising you’ll have
- The two incision are less than an inch long and closed with absorbable suture and the incisions take about two weeks to heal.
- Being up and about probably won’t hurt the repair of the vasectomy site inside or the healing process on the outside but extra swelling may slow the process and may make you more uncomfortable.
- We recommend no strenuous activity or sex for three weeks.
- Having said all of this I have had patients who told me they planned to go to work “a desk job” the next day
- And I have had a patient he had sex the night of the procedure-of note he came to the office the next day all “swollen up” and yet he and his wife were pregnant in three months. Go figure!
The last guy…he was practicing the art of getting away with it and got away with it. But…not everybody does.
I tell patients the “company policy” is off your feet as long as possible, the more you’re off your feet the less swelling and bruising, and no sex or strenuous activity for three weeks. However just like in companies, the company policy is rarely adhered to or enforced…it is a template of what is desirable.
Does steroids given pre and post vasectomy reversal improve the chances of pregnancy? A good question.
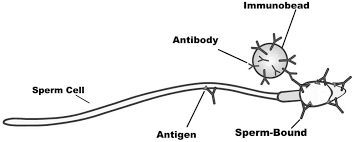
Reversal of vasectomy: the effects of sperm antibodies on subsequent fertility.
Abstract
Antisperm antibodies were measured in serum and seminal plasma in 130 males before and after vasectomy reversal and the occurrence of pregnancy was analysed in the partners of 77 who were followed for more than one year. Sperm-agglutinating antibodies were found in the serum of 79% of patients; seminal plasma antibodies were present in only 9.5% before reversal and this rose to 26% afterwards. Pregnancies occurred in the partners of 53% of those men who were trying to produce children. A pregnancy was significantly less likely when the pre-operative serum antisperm antibody titre was 512 or more, but no decrease in fertility was seen with titres below this. Several pregnancies were produced by patients with seminal plasma antibodies, but numbers and follow-up are too small to permit detailed analysis.
A randomised controlled trial of peri-operative steroids showed that they produced no benefit.
The antisperm antibodies associated with vasectomy reversal appear to differ fundamentally from those occurring in naturally subfertile males.
Vasectomy Reversal Success Depends on Three Big Things…Read On!

The three things…The surgeon, the quality of fluid at the time of the procedure, and the years since the vasectomy…and a little luck.
Time to Sperm Appearance Can Be Predicted After Vasectomy Reversal
Urology – November 30, 2007 – Vol. 23 – No. 08
Article Reviewed: The Kinetics of the Return of Motile Sperm to the Ejaculate After Vasectomy Reversal. Yang G, Walsh TJ, et al: J Urol; 2007; 177 (June): 2272-2276.
Can you achieve pregnancy after Vasectomy reversal and only one testicle?
Pregnancy with Vasectomy Reversal With One Testicle?

Vasectomy Reversal Pregnancy with one testicle: The above logo is a microbrewery company in our city and I thought the name lends itself to introduce this blog’s message. I should have been asked to be an investor!
Vasectomy Reversal Pregnancy with one testicle? Actually this question comes up often to the urologist. Patients lose a testicle for several reasons to include: chronic epididymitis, orchitis, undescended testicle, testicular cancer, trauma, and chronic pain. In the majority of cases having only one testicle does not affect fertility or male hormone production.
The reason we mention this here is that it does occasionally become an issue for the couple desiring a reversal. Can you reverse the vasectomy on one testicle and have success? Yes. Do you have a better chance of success after a reversal if you have two testicles? Yes.
Although the one testicle can produce the quality and quantity of sperm for pregnancy after a reversal, having two testicles results in a higher likelihood of success because there are two chances that the anastomosis (the repair of the vas deferens) remain open, two chances of having good fluid in the proximal (testicle side of the vas), and the benefit of two testicles contributing to the semen quality.
It is not unusual at the time of a reversal to have very good quality fluid on one side because of a sperm granuloma on that side, and on the other side the fluid is of poor quality i.e. cloudy with sperm parts and no whole sperm.
So…if we had our druthers, we’d want to begin with two testicles to work with, however it is reasonable to have a reversal if the patient only has one testicle.