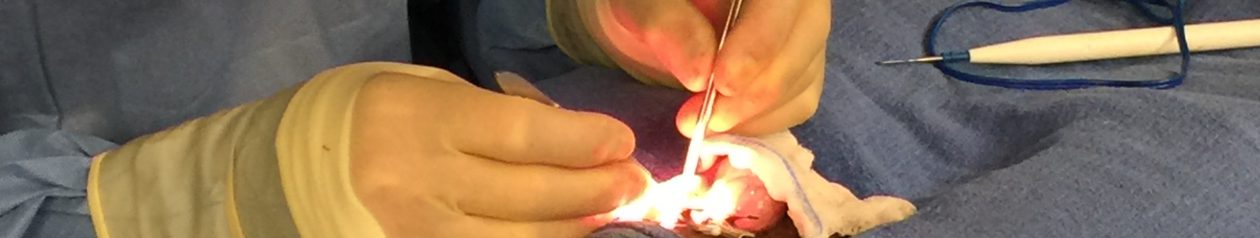
The vas deferens closest to the testicle and just before the epididymis is the convoluted portion of the vas. As you see above the vas then “straightens out” the further you get away from the testicle.
Above you see the “old vasectomy” site marked and it is in the mid scrotal area and in the straight not convoluted portion of the vas. This is the ideal location for the reversal doctor because it is away from the inguinal area and up from the smaller and more difficult to isolated convoluted portion.
Although you can feel the vasectomy site through the scrotal skin preoperatively, you really cannot tell where in the course of the vas it actually is.
Recently I performed a reversal and both sides of the vasectomy site were in the convoluted portion of the vas and close to the epididymis. This required more dissection to reach and it is tricky to get a portion of the convoluted vas to reconnect that is straight (as opposed to curved away from the other side of the vas).
So yes if the person who did the vasectomy happened to do it in the middle, that is away from the inguinal area as well as away from the convoluted portion of the vas then the procedure is much easier to locate, to prepare for the reversal, and to perform the reversal.
You might ask, “Why wouldn’t every urologist make a point to do the vasectomy in the best position in case a reversal has to be done years later.”
Well a reasonable enough question but there are two factors to consider as to why urologists don’t think this way.
- Vasectomies are usually done in the office under local anesthesia and depending on the patient and the patient’s scrotal anatomy…he gets the vas where he can get it…i.e. sometimes you can’t pick and choose a site the patient’s anatomy dictates that.
- Also, the vasectomy is supposed to be considered permanent and the primary goal is a good vasectomy and prevention of pregnancy. Vasectomies are not and probably should not be done with the idea in mind that the patient will reverse it.
- In my practice if I were asked to do the vasectomy so it could be more easily reversed, I’d probably tell the couple to re consider a vasectomy until they felt it was permanent and they had no plans for further children.
- Having said that, a urologist can try to make a point to be “in the middle” but as I mentioned sometimes you take the vasectomy site where the patient’s scrotum gives it to you.
Reversals Are What We Do.