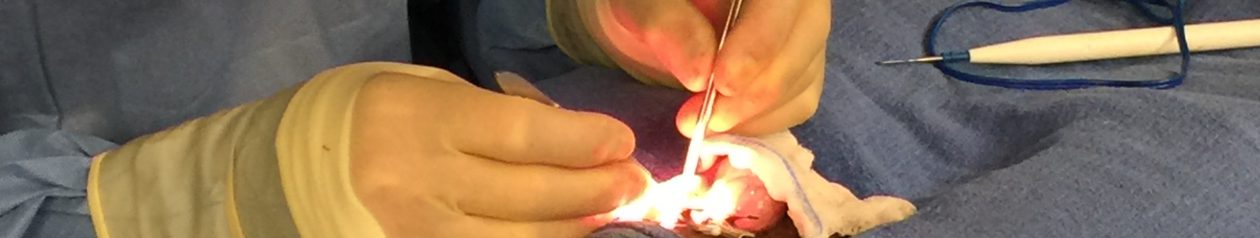
The following is from a vasectomy reversal doctor in England. The process is similar to but not exactly the same as at Georgia Vasectomy Reversal, however it is informative and adds to the data base of the couple contemplating a vasectomy reversal.
Vasectomy reversal myths debunked
If you’re too old, you can’t have a vasectomy reversal
The reality is, a vasectomy reversal can be performed at any age, so long as an individual is healthy enough to undergo the treatment.
A vasectomy reversal rarely works after 10 years
This is a popular misconception and is based on outdated studies. Modern techniques used today have increased the vasectomy reversal success rate even if the original vasectomy was performed years ago. Even after about 20 years, you still stand an 84% chance of success following a vasectomy reversal.
Anti-sperm antibodies cause infertility even after a vasectomy reversal
It is widely believed that anti-sperm antibodies attack healthy sperm following a reversal and can cause infertility. In actual fact, antibodies are present in the blood and not in sperm following a vasectomy reversal, so are normally not responsible for any fertility problems that may arise following the procedure.
IVF is a better option than vasectomy reversal
You will need to weigh up the pros and cons of choosing IVF or vasectomy reversal, but there are many benefits to choosing reversing a vasectomy over IVF. For starters, a vasectomy reversal is a quick, single procedure that has good success rates, enabling you to conceive a baby naturally. In contrast, IVF is a gruelling process that often requires several attempts to increase the chance of success. The cost of a vasectomy reversal is also much lower compared to IVF procedures. Bear in mind also that there is a greater chance of multiple pregnancies when opting for IVF, so if you are only hoping for one baby, a vasectomy reversal is easily a better option.
Vasectomy reversal successes are the same whoever you choose
This is not the case at all. Doctors and standards vary, so if you want to achieve the best results possible choose a surgeon who is specialised in vasectomy reversal and has extensive experience. Mr Harriss has many years of experience and is available to answer any questions that you may have.