Thank you Dr. McHugh! After our 3rd child was born my husband and I thought we were done having children and opted to have a vasectomy. Well, about a year later we both realized that we were not done having children and wanted to try for one more. I researched urologists in the area that performed vasectomy reversals and Dr. McHugh really stuck out to me. My husband had his consultation and agreed that he was a great doctor and felt really comfortable with him. My husband had his VR done October 30, 2014 and I was pregnant 4 months later. We couldn’t believe it and we were so ecstatic! Our perfect little girl, Layla Anne Kapish was born November 3, 2015 at 8lbs 6oz. Now with two girls and two boys she really completes our family and we couldn’t imagine life without her. If you are considering a vasectomy reversal, Dr. McHugh is the one you should see. We HIGHLY recommend him! Thank you so much again to him and all of his staff. INCREDIBLE!
Sincerely,
Marly and Robert Kapish
Tag Archives: vas reversal cost
Why doesn’t the average urologist do vasectomy reversals?
Most urologists do a vasectomy once or twice a week. They can be done in the office and usually take fifteen minutes or so to do. We call that in the business a “bread and butter” procedure. In other words, a vasectomy is something that most urologists do often and well. (I might add that some urologists do a better job than others in this procedure-that is true for most surgical specialties.)
Since only about 1 in 6 men who have had a vasectomy will, at some point due to a change in his circumstances consider a reversal, several factors come into play that dissuades the urologist from agreeing to perform the procedure.
- Fewer numbers of available men wanting the procedure for the average urologist to become proficient in performing it.
- The procedure takes around 2-3 hours to perform and done looking through a microscope throughout the procedure.
- It is not covered by insurance-some patients want a reversal but can’t afford it.
- There is a steep learning curve in doing the procedure well and in a timely fashion.
- There are expected results by the patient who will be inconvenienced, undergo a surgical procedure and at an expense not covered by his insurance. (When a general surgeon removes the gallbladder, well he removes it…it is not like some function will be expected beyond that. The reversal couple rightfully expect and hope that there will be sperm in the ejaculate after the reversal. This is a lot for the average urologist who would much rather just send the patient desirous of a reversal to someone “Who does them all the time.” Let him or her deal with all the expectations and potential of having put someone through all this and then no sperm in the ejaculate.)
- The procedure requires special instruments, an operating microscope, and special suture. The local hospital may or may not have all this and if they do, then the patient has the added expense of the hospital fees making the patient pay at a premium for the “set up” and by a urologist who does the procedure infrequently.
- Not all physicians are comfortable or have the skills to use microscopic suture and to sew and tie suture under the microscope. Without this skill set, the 2-3 hour procedure can last much longer with less acceptable results.
- So…that the average urologist doesn’t do this procedure is a good thing and how it should be. If they aren’t comfortable with the procedure and logistics of it they shouldn’t be doing it.
It is a fair question for the patient to ask their doctor, “Do you do this procedure commonly?” “How many have you done?”
At Northeast Georgia Urological Associates we have an accredited surgery center appropriately equipped for this procedure, we are approaching 130 reversals done and our patency rates compares favorably with studies in the medical literature.
On top of that-we enjoy performing the procedure, the hopeful couples, and the happy results.
We look forward to working with you!
The major factors in a successful vasectomy reversal. John McHugh M.D.
- The age of the male.
- The age of the female.
- The time since the vasectomy.
- The quality of the sperm from the testicular end of the transected vas at the time of the reversal procedure.
- The technical quality of the reversal procedure itself and the experience of surgeon.
- Some degree of luck for all of these factors to come together and result in pregnancy.
Post Vasectomy Pain Syndrome: Reason for Vasectomy Reversal?
I have done over a thousand vasectomies and to my knowledge have not seen this syndrome in my practice.
Having said that, I do believe this malady does exist. But here is the thing, when a patient has a vasectomy reversal to alleviate the pain, it may not be the reversal per se that makes the pain go away.
I recently did a vasectomy reversal on a patient that wanted the procedure to have another child. He did, however, mention that he was told that clips were used for his vasectomy and that he had had pain in the right testicle since the procedure. At the time of the reversal on the right side I found a sperm granuloma (an inflammatory mass in the area of the vasectomy as a result of the body’s attempt to correct the trauma of the surgery and response to sperm which the body views as a foreign body) and marked surrounding inflammatory changes. There were clips noted and dissecting the granuloma out, cleaning the two ends of the vas and removing the “inflammatory glob” was more difficult than the usual dissection. So at the end of the reversal on the right side the patient had the granuloma removed and pristine ends of the vas reconnected with microscopic suture.
It is too early to say if the reversal in terms of pregnancy and patency was successful. But what if his right testicular pain goes away? Maybe it is the removal of the sperm granuloma and not reconstituting the vas. In other words a vasectomy reversal done of post vasectomy pain syndrome that is successful, might have been because of removing the scar tissue and not the reversal.
I had a reversal patient several months ago tell me as he was leaving our surgery center that the primary reason for having the reversal was for pain and not children. He failed to tell me that preoperatively and if he had I would have discouraged having a reversal for that purpose alone. (Surgeon’s rule number one: Don’t operate on folks for pain.) As it turned out, he wrote me a note complimenting my staff at our surgery center and that he was very pleased with the results, i.e. no more pain not that there was a pregnancy.
In summary, there may be something to having a reversal to alleviate chronic post vasectomy pain but it may have more to do with removing the sperm granuloma and inflammatory tissue than restoring the flow of sperm.
Birth defects after microscopic vasectomy reversal?
Just like the Marines…only the strongest, the fastest, the finest “get through.” And this is natures way of assuring the best sperm for the job.
“Cracking the egg” is very competitive!
A link between vasectomy reversals and birth defects has not been convincingly demonstrated.
Considering a vasectomy reversal? Consultation is free.

If you are considering a vasectomy reversal, even if you are unsure who you will choose to perform it, it is a good idea to have a preoperative consultation. You can ask the pressing questions that concern you, you can get a concept of the procedure, the time it will take, the cost, and as a result of the exam of the previous vasectomy site-you will know if there are any contraindications for the procedure pertinent to you. It is also an opportunity to get to know the physician that may be doing the procedure.
The reason it is not unusual for a consultation to be free for reversals is that the visit and the subsequent procedure is usually not covered by insurance. The free consultation is beneficial to both parties and by being at no cost encourages the couple to take that”first step” to the journey of having another baby.
How long after microscopic vasectomy reversal can a couple have sex?
Answer: One month is the usual recommendation however, I have had couples tell me (I am not making this up) that they had sex the evening of the procedure and that the reversal resulted in a baby.
The microscopic reversal is watertight from the microscopic sutures (meaning conceivably that tube is patent from the get go and that sperm can traverse the reversal without leakage) however there are other areas of the procedure that need to heal as well. So the one month of waiting is for everything to heal properly- from the skin incision, to the vessels that surround the vas deferens and the repair itself.
Is the No Scalpel Vasectomy a gimmick? Yes and No.
The very first vasectomy ever performed probably isolated the vas deferens, cut out a section and then destroyed the cut ends. This has the effect of a double whammy to assure sterility. How the ends are destroyed or closed is myriad-clips, suture, fulguration, folding the vas on itself and tying- doesn’t really matter in terms of the long-term success rates.
When I learned to do a vasectomy as a resident in the 1980’s, we made a fourth of an inch midline scrotal incision and brought the vas to the surface with a instrument called a towel clip. It had two fine pointed ends and was used to hold towels in place to isolate the surgical field. This instrument was adapted to many functions in surgery and in urology was the device of choice for a vasectomy.
The China Method or the No scalpel method introduced two instruments. One is the fine pointed hemostat which is used to spread the skin for the vasectomy opening. (So there is still an opening but you did not use a scalpel to make it-whoopee do.)
The fine pointed hemostat is also used to open the vas sheathing without having to incise it with a knife once the vas has been isolated and brought to the skin.
This is where the grasper is used. The opening is smaller-a grain of rice in length- and the grasper allows for the urologist to easily grasp and bring the vas to the skin to perform the procedure.
The story line goes that the procedure has a smaller opening, that the opening heals better because the skin has been spread and not cut, the procedure can be done quicker because of these instruments, and that the patients do better with less heal time and fewer complications.
So is it a gimmick? Well it is a better procedure now because of these instruments, but we still identify, cut and destroy. You can decide if all this fuss in nomenclature warrants “spreading” is better than “cutting” an opening that is less than a centimeter in length.
No Scalpel does have a ring to it I must admit. The No Needle vasectomy is another story; I’ll do that at another time.
Of note, these same two instruments are also very useful in preparing the post vasectomy vas for the microscopic vasectomy reversal.
Atlanta Ga:Why do Vasectomy Reversals cost more than vasectomies?

Atlanta, Ga Vasectomy Reversal Cost: Cutting the vas deferens in two (a vasectomy) is easier than putting it back together (a vasectomy reversal) and is indeed a horse of a different color.
Atlanta, Ga Vasectomy Reversal Cost:
- Vasectomies are covered by insurance-vasectomy reversals are not.
- Because the reversal is not covered by insurance, the patient pays the entire expense of the procedure – the surgeon, staffing, operating microscope, supplies (microscopic suture) and the facility.
- The reversal all-inclusive is relatively high because the surgeon becomes the hospital. All the fees associated with this procedure are paid by the surgeon.
- Only a small percentage of urologists perform microscopic vasectomy reversals at all and even less perform this procedure commonly.
- The procedure requires identification of the vasectomy site and preparing it for the reversal. Microscopic suture and an operative microscope is utilized to accomplish the reversal. To perform this procedure effeciently and effectively requires skill and years of experience.
- Some urologists perform the procedure in an office setting with local anesthesia. Because this does not require an accredited facility and an anesthesiologist, these physicians are able to perform a reversal at a lower price. (The patient does not have the option of I.V. anesthesia for the 2-3 hour procedure.)
- Urologists who work exclusively through a hospital and use the hospital operating room usually have the highest total reversal cost.
- Urologists who use general anesthesia and an independent ambulatory surgery center pays the center for the anesthesia, materials and staffing. The fee of the urologist then is added to this for the all inclusive cost of the procedure.
- We own our accredited surgery center and are licensed for general anesthesia. In this scenario, the surgeon has more options regarding costs. Owning the surgery center cuts out the middle man of a hospital or an independent surgery center. This results in a lower cumulative price but with the benefits of a hospital. The cost of a reversal in this scenario represents a blend of the most expensive hospital based procedure and the least expensive (only oral medications and local needle anesthesia) office based procedure.
- Just because a surgeon charges more for a reversal doesn’t mean he or she is better qualified to perform the reversal. There may be other costs involved that the surgeon must account for in his pricing that have nothing to do with his surgical fee or skill in performing the procedure, i.e the facility, the microscope, the suture, anesthesia, and the staffing.
- Because a reversal is not covered by insurance, the surgeon bundles all of the costs associated with the procedure so that the patient only has one fee.
- The above makes the reversal procedure expensive and the expense more noticeable because the patient must pay out of pocket.
- This in turn highlights why urologists are hesitant to say they can do a reversal despite having little experience to do the procedure because the patient and the doctor are both very disappointed when the procedure isn’t successful. It would be somewhat disingenuous for a doctor to charge a patient the fees, put him through a surgical procedure and knowing he has very little experience in the procedure. A physician saying “I can do a reversal” is different from one who performs them weekly.
- This thought process also limits urologists agreeing to do a reversal for concerns of doing the procedure poorly and with poor results. With a reversal, there is the procedure itself and then there are functional expectations, i.e. the presence of sperm and pregnancy.
- Just as with any surgical procedure, the due diligence and decision making is the responsibility of the patient and his family. As a result, all of the factors noted above should be taken into consideration.
- Patients need to know from the start what they are getting into and that despite everything going just right there is a percentage of patients who don’t achieve pregnancy. (Success depends on the skill and experience of the surgeon, the time from the vasectomy and the quality of the fluid at the time of the reversal.)
- All of the above caveats, which are unique to a microscopic vasectomy reversal are discussed at length during the free reversal phone consultation and, as well on our website. Gavasectomyreversal.com
Summary: This is why there is variance in the cost of a reversal, why it is harder to perform, why only few urologists do commonly, and why more skill, resources and expense are required than a vasectomy.
Vasectomy Reversals are What We Do!
Vasectomies and reversals performed by Dr. McHugh since 2020!
Vasectomies
Vas Reversals
Vasectomies and Reversals
Vasectomy Reversal: Patency vs. Pregnancy-A big difference.
After a microscopic vasectomy reversal, several factors come into play that determine pregnancy. The technical aspects of the procedure must succeed. The surgeon, by experience and care to assure a watertight and tension free anastamosis, hopefully will give the patient the best chance of “having an open vas tube.”
If the reversal is successful and the tube is open, then it is the patient’s testicles turn to “man up.” The longer interval between the vasectomy and the reversal the less likely the testicles have the ability to “pick up the ball” and begin to produce normal sperm that have the ability to be motile. (No pun intended.) The longer the interval, the longer it takes the testicles to produce sperm that can get the job done. This is an imponderable; as no one knows before the reversal the potential of the testicles ability to produce sperm suitable for pregnancy.
So let’s say the reversal is perfect and sperm produced by the testicles are getting through the old vasectomy site are viable, strong, and very motile. Well then, there are the normal things that hinder pregnancy that normal couples, neither of which have had any procedure, experience.
After all this and surmounting the odds of the procedure, the testicles producing good sperm, the length of time since the reversal and the things that are sometimes difficult in pregnancy in the normal situation, pregnancy occurring is much lower percentage than the presence of sperm in the post reversal ejaculate.
This is why the couple considering a vasectomy reversal, and the attendant inconvenience and expense, need to be aware of the difference between patency and getting pregnant.
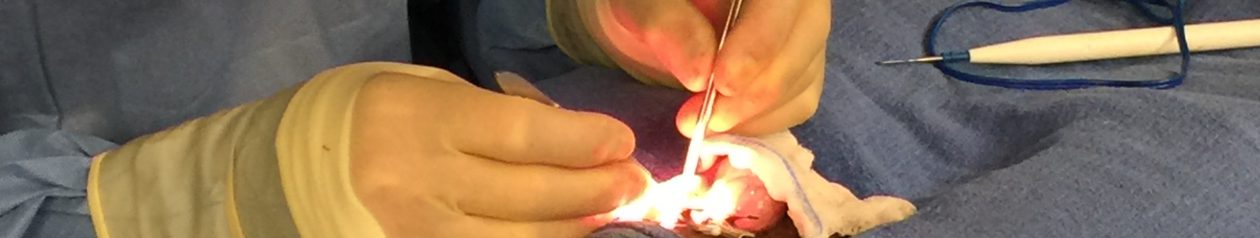
























































 Vasectomy Reversal
Vasectomy Reversal






































